Chagas Disease
Chagas disease is a neglected tropical disease caused by the protozoan parasite Trypanosoma cruzi. Parasite transmission occurs through direct interaction with an infected triatomine insect vector known as the “kissing bug”. The fecal material of the bug carries the parasite which can enter the skin of the bite or contaminate food products leading to oral ingestion. Another route is congenital infection where an infected mother can pass the parasite to her unborn fetus. Less common routes of infection include a contaminated blood transfusion (usually before 2007 in the United States and in countries that do not screen for Chagas) and organ transplantation in a donor who was not screened for Chagas but infected and donates their organs.
Pictured below are common Kissing Bugs found in Central and South America that are known vectors of Chagas disease.

Chagas disease is a chronic infection that often goes unrecognized for decades because the vast majority of those infected are asymptomatic at the time they acquire the parasite. Some will not develop a disease from the infection, but approximately 30-40% will eventually manifest chronic illness which can be life-threatening. Chagas heart disease is the most commonly affected organ which can lead to progressive heart failure, abnormal heart beats and rhythms, and possibly sudden cardiac arrest. Another area of the body affected is the gastrointestinal tract. This can cause problems with swallowing food and liquids, digestion, and defecation of stool. The esophagus and colon can sometimes become enlarged and trigger debilitating gastrointestinal manifestations.
There are three phases to this infectious process:
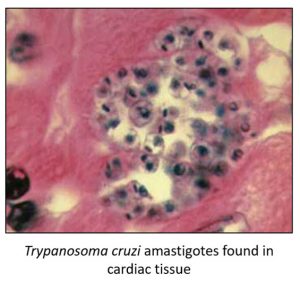 Acute phase:
Acute phase:
- Time of infection the majority will not have symptoms
- If symptoms develop usually non-specific; fever, enlarged lymph nodes, fatigue
- These non-specific symptoms can last for day to weeks but then resolve
- Chagoma is local inflammation at the site where the parasite entered the skin (can easily be confused with allergy to Kissing bug bite)
- Remember the Kissing Bug bite DOES NOT transmit the parasite; only the fecal matter of the bug contains the parasite and the kissing bug will need to defecate on you during feeding for transmission to occur if related to a bite.
- Romaña’s sign: swelling around the eye of a person who contracted the parasite through the mucous membranes (not common)
- If a person has an existing weakened the immune system they can develop a serious acute infection such as myocarditis (inflammation of the heart), pericardial effusion (fluid around the heart) and even meningoencephalitis (swelling of the brain and lining).
After acute infection we do not know who will clear the infection naturally or who will develop a chronic illness. Unfortunately the testing that is currently available can only determine if you have had exposure to the parasite. These tests primarily look at antibodies (memory proteins produced by certain immune cells in the blood) created against T. cruzi. Sometimes we can detect the parasite through microscopy of blood or tissue samples or other molecular techniques utilized to detect T. cruzi DNA.
This is where things sometimes can get confusing but let’s dive in deeper. If you screen positive and then have positive confirmatory testing done that is specific for exposure to T. cruzi, then you have been exposed and are deemed infected. Since we do not have a test that tells us if you may or may not develop a chronic illness from the parasite, and you do not have any clinical evidence of a disease related to Chagas, you are now classified as being in the “indeterminate phase”.
Indeterminate Phase:
- Do not have any clinical evidence of an illness related to Chagas disease
- Screening and confirmatory testing is positive for exposure to the parasite
- Majority of people will remain without symptoms in their life but sometimes parasite can be detected intermittently in the blood
- If a person develops a condition that weakens the immune system (AIDS, blood cancer, chemotherapy, immune suppressing agents for organ transplantation…) then the parasite can “reactivate” and then cause a serious disease which is sometimes fatal
- People with indeterminate phase of Chagas disease should be monitored with a clinical provider for the development of Chronic Chagas disease.
Chronic Phase:
Chagas heart disease: most common organ involved.
- Will typically lead to abnormal electrical activity (heart block, arrhythmias…)
- Sudden cardiac arrest does occur
- Dilated cardiomyopathy and congestive heart failure (weakened heart)
- Typically take 2-3 decades to clinically recognize heart involvement
Gastrointestinal tract disease: abnormal swallowing and enlargement of esophagus and/or colon
- Progressive trouble swallowing liquids then solids are typically first
- Chronic constipation and abdominal pain; colon will sometimes perforate
- Colon can enlarge and distend the abdomen
Thromboembolic disease: higher rates of pulmonary embolism and stroke have been described among those with chronic Chagas disease.
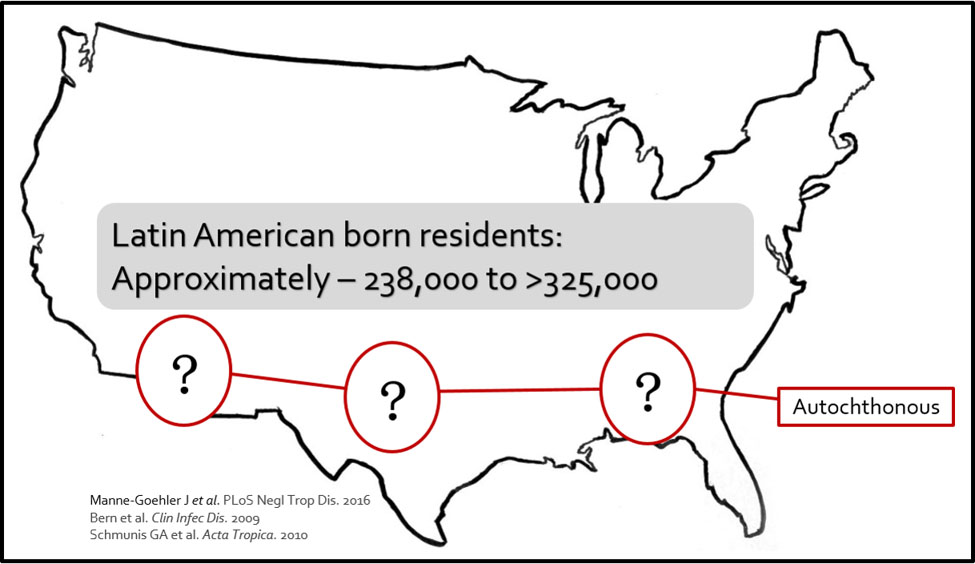
Chagas disease is endemic in 21 Latin American countries (excluding the Caribbean islands) with approximately 70 million people at-risk for this parasitic infection. Seven million people are estimated to be infected from endemic regions living throughout the world with an estimated 10,000 deaths occurring each year within the Americas. The United States Centers for Disease Control and Prevention suggest that greater than 300,000 people in our country are infected but less than 1% have actually been diagnosed. Florida is estimated to carry the third highest burden with 18,000 individuals living with the disease. Locally acquired (autochthonous) cases of Chagas disease have been confirmed or suspected in the United States and reported in California, Arizona, Texas, Louisiana, Tennessee, and Mississippi. However these are sporadic cases and transmission dynamics amongst an at-risk population has not been studied and more research is needed to better understand the kissing bugs found here naturally in the United States.
Chagas Disease Testing, Treatment and Management
Chagas disease testing can be arranged by your primary care provider or a specialist who focuses on infectious diseases. Antiparasitic medications are also available in the United States for those who qualify for such treatment. Clinical management and referrals to specialists who care for those with Chagas disease can be arranged from your primary care provider.

If you live in Florida and would like to learn more about Chagas disease research being conducted please email our Research Team: Chagas-disease@ufl.edu
Please visit the “Research” tab to learn more about Kissing Bug and Chagas Disease research projects!


